Before contracting COVID-19 in March, Beth Moore was doing group workouts, running around with her kids, and working hard as an attorney. Her symptoms lasted through April and went away. But in May, her mind and body went haywire.
"I was truly convinced I was having some sort of mini stroke or a heart attack," she recalled to Newsy.
And it didn’t go away.
"I found that even with, you know, simple things like having conversations with my kids. I'm forgetting words like I'm saying. I'm talking about the refrigerator. But I'm saying go get a drink out of the. And I can't find the word for a refrigerator in my head, which is bizarre, that just never happened to me before," she said.
Tasha Crabtree first got sick in March. She also has been fighting what she calls "COVID brain."
"I can sit here and have a coherent conversation with you. And then halfway through a sentence, I will forget a word and I will focus so hard on that word that I completely forget my train of thought," she said.
The women are among the estimated one-third of COVID-19 patients who experience neurological complications. It often shows up as a struggle to think or a lapse in memory.
"I'm sorry. I find it very difficult to describe what it actually feels like. But it's it's like. Let's see," Crabtree paused and laughed. "Well, here's an example. I have lost my train of thought."
Now, clinics are popping up specifically for patients like these two. Dr. Igor Koralnik is the chief of Neuroinfectious Diseases and Global Neurology at Northwestern Medicine. His Neuro COVID-19 clinic in Chicago is swamped with patients from all 50 states.
"We are in high demand. There are, you know, many more patients that we can see, you know, even if we were going to be 24/7," Koralnik told Newsy.
Somes symptoms are mild, like those experienced by Beth Moore and Tasha Crabtree. Koralnik says he’s also seen COVID-19 patients develop stroke, seizures, or paralysis, and mental health disorders.
A new Oxford study found COVID-19 patients with no prior psychiatric history had an increased rate of psychiatric diagnoses the three months after infection.
"Why this virus causes all those problems is not entirely known at this point," Koralnik said.
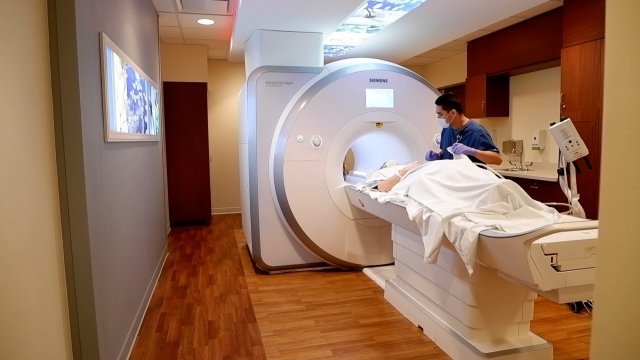
Koralnik uses MRI’s to measure the impact COVID has on the brain. Some patients take an NIH-developed cognition test that lasts about 30 minutes. They’ll come back a few months from now to examine if the tests show any decline that could give clues about long-term effects.
There’s individual stories from patients of little wins. For Tasha Crabtree, it included going back to work in her Nevada vet office.
"I was able to do some of the more difficult aspects of my job without mistakes, without error. And so it does feel good," she told Newsy.
But the big question remains, what will long-term brain impacts be?
"I hope that a patient with a minor brain fog will go back to full recovery over time, but it's too early to tell," Koralnik said.
"I'm hopeful that we’ll eventually get back to our normal baseline. That's my hope. That's my goal. That's what I want. But the fear that's in the back of my head is that this is my new reality," Moore said.